We all evolved from one single-celled organism that lived billions of years ago. I don’t see why this is so hard for some people to believe, given that all of us also developed from a single fertilized cell in just 9 months.
However, our most recent common ancestor is not that first single-celled organism, nor is it the first Homo sapiens, or even the first Cro-Magnon.
The majority of the people who read this blog probably share a common ancestor who lived no more than 640 years ago. Genealogical records often reveal interesting connections - the figure below has been cropped from a larger one from Pinterest.
You and I, whoever you are, have each two parents. Each of our parents have (or had) two parents, who themselves had two parents. And so on.
If we keep going back in time, and assume that you and I do not share a common ancestor, there will be a point where the theoretical world population would have to be impossibly large.
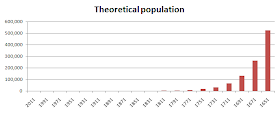
Assuming a new generation coming up every 20 years, and going backwards in time, we get a theoretical population chart like the one below. The theoretical population grows in an exponential, or geometric, fashion.
As we move back in time the bars go up in size. Beyond a certain point their sizes go up so fast that you have to segment the chart. Otherwise the bars on the left side of the chart disappear in comparison to the ones on the right side (as several did on the chart above). Below is the section of the chart going back to the year 1371.
The year 1371 is a little more than 640 years ago. (This post is revised from another dated a few years ago, hence the number 640.) And what is the theoretical population in that year if we assume that you and I have no common ancestors? The answer is: more than 8.5 billion people. We know that is not true.
Admittedly this is a somewhat simplistic view of this phenomenon, used here primarily to make a point. For example, it is possible that a population of humans became isolated 15 thousand years ago, remained isolated to the present day, and that one of their descendants just happened to be around reading this blog today.
Perhaps the most widely cited article discussing this idea is this one by Joseph T. Chang, published in the journal Advances in Applied Probability. For a more accessible introduction to the idea, see this article by Joe Kissell.
Estimates vary based on the portion of the population considered. There are also assumptions that have to be made based on migration and mating patterns, as well as the time for each generation to emerge and the stability of that number over time.
Still, most people alive today share a common ancestor who lived a lot more recently than they think. In most cases that common ancestor probably lived less than 640 years ago.
And who was that common ancestor? That person was probably a man who, due to a high perceived social status, had many consorts, who gave birth to many children. Someone like Genghis Khan.
Wednesday, December 27, 2023
Monday, October 23, 2023
The Friedewald and Iranian equations: Fasting triglycerides can seriously distort calculated LDL
Standard lipid profiles provide LDL cholesterol measures based on equations that usually have the following as their inputs (or independent variables): total cholesterol, HDL cholesterol, and triglycerides.
Yes, LDL cholesterol is not measured directly in standard lipid profile tests! This is indeed surprising, since cholesterol-lowering drugs with negative side effects are usually prescribed based on estimated (or "fictitious") LDL cholesterol levels.
The most common of these equations is the Friedewald equation. Through the Friedewald equation, LDL cholesterol is calculated as follows (where TC = total cholesterol, and TG = triglycerides). The inputs and result are in mg/dl.
LDL = TC – HDL – TG / 5
Here is one of the problems with the Friedewald equation. Let us assume that an individual has the following lipid profile numbers: TC = 200, HDL = 50, and TG = 150. The calculated LDL will be 120. Let us assume that this same individual reduces triglycerides to 50, from the previous 150, keeping all of the other measures constant with except of HDL, which goes up a bit to compensate for the small loss in total cholesterol associated with the decrease in triglycerides (there is always some loss, because the main carrier of triglycerides, VLDL, also carries some cholesterol). This would normally be seen as an improvement. However, the calculated LDL will now be 140, and a doctor will tell this person to consider taking statins!
There is evidence that, for individuals with low fasting triglycerides, a more precise equation is one that has come to be known as the “Iranian equation”. The equation has been proposed by Iranian researchers in an article published in the Archives of Iranian Medicine (Ahmadi et al., 2008), hence its nickname. Through the Iranian equation, LDL is calculated as follows. Again, the inputs and result are in mg/dl.
LDL = TC / 1.19 + TG / 1.9 – HDL / 1.1 – 38
The Iranian equation is based on linear regression modeling, which is a good sign, although I would have liked it even better if it was based on nonlinear regression modeling. The reason is that relationships between variables describing health-related phenomena are often nonlinear, leading to biased linear estimations. With a good nonlinear analysis algorithm, a linear relationship will also be captured; that is, the “curve” that describes the relationship will default to a line if the relationship is truly linear (see: warppls.com).
The Iranian equation yields high values of LDL cholesterol when triglycerides are high; much higher than those generated by the Friedewald equation. If those are not overestimations (and there is some evidence that, if they are, it is not by much), they describe an alarming metabolic pattern, because high triglycerides are associated with small-dense LDL particles. These particles are the most potentially atherogenic of the LDL particles, in the presence of other factors such as chronic inflammation.
In other words, the Iranian equation gives a clearer idea than the Friedewald equation about the negative health effects of high triglycerides. You need a large number of small-dense LDL particles to carry a high amount of LDL cholesterol.
An even more precise measure of LDL particle configuration is the VAP test; this post has a discussion of a sample VAP test report.
Reference:
Ahmadi SA, Boroumand MA, Gohari-Moghaddam K, Tajik P, Dibaj SM. (2008). The impact of low serum triglyceride on LDL-cholesterol estimation. Archives of Iranian Medicine, 11(3), 318-21.
Yes, LDL cholesterol is not measured directly in standard lipid profile tests! This is indeed surprising, since cholesterol-lowering drugs with negative side effects are usually prescribed based on estimated (or "fictitious") LDL cholesterol levels.
The most common of these equations is the Friedewald equation. Through the Friedewald equation, LDL cholesterol is calculated as follows (where TC = total cholesterol, and TG = triglycerides). The inputs and result are in mg/dl.
LDL = TC – HDL – TG / 5
Here is one of the problems with the Friedewald equation. Let us assume that an individual has the following lipid profile numbers: TC = 200, HDL = 50, and TG = 150. The calculated LDL will be 120. Let us assume that this same individual reduces triglycerides to 50, from the previous 150, keeping all of the other measures constant with except of HDL, which goes up a bit to compensate for the small loss in total cholesterol associated with the decrease in triglycerides (there is always some loss, because the main carrier of triglycerides, VLDL, also carries some cholesterol). This would normally be seen as an improvement. However, the calculated LDL will now be 140, and a doctor will tell this person to consider taking statins!
There is evidence that, for individuals with low fasting triglycerides, a more precise equation is one that has come to be known as the “Iranian equation”. The equation has been proposed by Iranian researchers in an article published in the Archives of Iranian Medicine (Ahmadi et al., 2008), hence its nickname. Through the Iranian equation, LDL is calculated as follows. Again, the inputs and result are in mg/dl.
LDL = TC / 1.19 + TG / 1.9 – HDL / 1.1 – 38
The Iranian equation is based on linear regression modeling, which is a good sign, although I would have liked it even better if it was based on nonlinear regression modeling. The reason is that relationships between variables describing health-related phenomena are often nonlinear, leading to biased linear estimations. With a good nonlinear analysis algorithm, a linear relationship will also be captured; that is, the “curve” that describes the relationship will default to a line if the relationship is truly linear (see: warppls.com).
The Iranian equation yields high values of LDL cholesterol when triglycerides are high; much higher than those generated by the Friedewald equation. If those are not overestimations (and there is some evidence that, if they are, it is not by much), they describe an alarming metabolic pattern, because high triglycerides are associated with small-dense LDL particles. These particles are the most potentially atherogenic of the LDL particles, in the presence of other factors such as chronic inflammation.
In other words, the Iranian equation gives a clearer idea than the Friedewald equation about the negative health effects of high triglycerides. You need a large number of small-dense LDL particles to carry a high amount of LDL cholesterol.
An even more precise measure of LDL particle configuration is the VAP test; this post has a discussion of a sample VAP test report.
Reference:
Ahmadi SA, Boroumand MA, Gohari-Moghaddam K, Tajik P, Dibaj SM. (2008). The impact of low serum triglyceride on LDL-cholesterol estimation. Archives of Iranian Medicine, 11(3), 318-21.
Thursday, August 17, 2023
Do prominent health gurus live longer?
Many years ago, when I started blogging about health issues, I noticed a couple of interesting patterns. The first pattern is that prominent health “gurus” often talk about having had serious health problems in their past, which they describe as having motivated them to do research on health issues – and thus become health gurus. Frequently these problems pop up before 45 years of age; this is a threshold beyond which there is a clearly noticeable increase in severity of health problems.
In fact, I remember being somewhat surprised by one such “guru” (I will not name him), who would regularly write posts saying something to the effect that “… finally, my health is now on the right track …” In other words, every few months or so this person had to deal with serious health problems, always coming up with reasonable knowledge-based solutions. The knowledge seemed to be of good quality, but this guy’s health was poor to say the least.
The second pattern, related to the above, is that prominent health gurus seem to have a below average life expectancy. The life expectancy for the general population is around 79 years of age in the USA at the time of this writing, according to the World Health Organization (). Anthony Colpo has written an interesting post about this below average life expectancy pattern among health gurus ().
To better understand and illustrate this situation to our blog’s readers, I created a dataset with 100 records, corresponding to 100 health gurus, with various variables interacting in ways that reflect the above observations. The observations are summarized as assumptions, listed later. The following variables are on a scale from 1 to 7; in real life they would have been measured retrospectively, looking back at a guru’s entire life:
- The guru's health before age 45 (BEF45).
- The guru's knowledge about health issues (KNOWL).
- The guru's health after age 45 (AFT45).
- The guru's prominence (GPROM).
Finally, the variable below is on a continuous scale of years, with an average of 79 and a standard deviation of 10. As mentioned earlier, 79 is the life expectancy for someone living in the USA at the time of this writing. The standard deviation of 10, which approximates that figure in the USA, means that approximately 68 percent of the individuals in the simulated dataset will have a life expectancy between 69 and 89. That is 79-10 and 79+10, respectively.
- The guru's age at the time of death (GAGED).
This experimental exercise with simulated data can be seen as a simulation “game”, where various variables interact to generate results that are not obvious. A widely used process to create data is known as the Monte Carlo method (), which is what we used here. I also made the following assumptions in the data creation process:
- That the poorer is the guru's health before age 45 (BEF45), the greater is the guru's knowledge about health issues (KNOWL). The reason for this is that poor health compels the person to study about health issues.
- That the poorer is the guru's health before age 45 (BEF45), the poorer is the guru's health after age 45 (AFT45). This assumes that the person has an underlying condition that causes the poor health in the first place, and that can be exacerbated by a poor diet and lifestyle.
- That the greater is the guru's knowledge about health issues (KNOWL), the better is the guru's health after age 45 (AFT45). This counteracts the effect above, and assumes that the knowledge is put to good use and contributes to improving the person’s health.
- That the greater is the guru's knowledge about health issues (KNOWL), the greater is also the guru's prominence (GPROM). In other words, a guru’s status among followers is enhanced by the guru’s knowledge.
- That the better is the guru's health after age 45 (AFT45), the higher is the guru's age at the time of death (GAGED).
A final assumption made is that the causal relationships laid out above have a small effect size (more technically, that they are associated with f-squared coefficients slightly below 0.1), meaning that random influences are not only present but also play a big role in what happens in the simulation. The causality links are summarized in the graph below, created with WarpPLS (). We also used this software to analyze the data.
Note that in our simulated data the guru's prominence (GPROM) does not directly influence the guru's age at the time of death (GAGED). Stated differently, there is no causality link between GPROM and GAGED, one way or the other, even though these two variables are likely to be correlated due to the network of causality links in which they exist. Nevertheless, it is by looking at the relationship between these two variables, GPROM and GAGED, that we can answer the question in the title of this post: Do prominent health gurus live longer?
And the answer appears to be “no” in our simulation. The plot below shows the relationship between a guru's prominence (GPROM), on the horizontal axis, and the guru's age at the time of death (GAGED), on the vertical axis. Each data point refers to a guru. On average, the greater a guru's prominence, the lower seems to be the guru’s life expectancy. Each one-point increase in prominence is associated, on average, with approximately a one-year decrease in life expectancy.
Note that there is one very prominent guru whose age at the time of death was around 95; the data point at the top-right corner (GPROM=7, GAGED~95). This happened largely by chance in our data. Nevertheless, assuming that our data somewhat reflects what could happen in real life, the followers of the guru would probably point at that longevity as being caused by the guru’s knowledge about health issues. They would likely be wrong.
Our dataset also allows us to estimate the probability that a fairly prominent guru (GPROM greater than 4, on a 1-7 scale) would have a below average life expectancy (GAGED lower than 79). That conditional probability would be approximately 60 percent.
Tuesday, February 28, 2023
Is heavy physical activity a major trigger of death by sudden cardiac arrest? Not in Oregon
The idea that heavy physical activity is a main trigger of heart attacks is widespread. Often endurance running and cardio-type activities are singled out. Some people refer to this as “death by running”.
Good cardiology textbooks, such as the Mayo Clinic Cardiology, tend to give us a more complex and complete picture. So do medical research articles that report on studies of heart attacks based on comprehensive surveys.
Reddy and colleagues (2009) studied sudden cardiac arrest events followed by death from 2002 to 2005 in Multnomah County in Oregon. This study was part of the ongoing Oregon Sudden Unexpected Death Study. Multnomah County has an area of 435 square miles, and had a population of over 677 thousand at the time of the study. The full reference to the article and a link to a full-text version are at the end of this post.
The researchers grouped deaths by sudden cardiac arrests (SCAs) according to the main type of activity being performed before the event. Below is how the authors defined the activities, quoted verbatim from the article. MET is a measure of the amount of energy spent in the activity; one MET is the amount of energy spent by a person sitting quietly.
- Sleep (MET 0.9): subjects who were sleeping when they sustained SCA.
- Light activity (MET 1.0–3.4): included bathing, dressing, cooking, cleaning, feeding, household walking and driving.
- Moderate activity (MET 3.5–5.9): included walking for exercise, mowing lawn, gardening, working in the yard, dancing.
- Heavy activity (MET score ≥6): included sports such as tennis, running, jogging, treadmill, skiing, biking.
- Sexual activity (MET score 1.3): included acts of sexual intercourse.
What did they find? Not what many people would expect.
The vast majority of the people dying of sudden cardiac arrest were doing things that fit the “light activity” group above prior to their death. This applies to both genders. The figure below (click to enlarge) shows the percentages of men and women who died from sudden cardiac arrest, grouped by activity type.
Sudden cardiac arrests were also categorized as witnessed or un-witnessed. For witnessed, someone saw them happening. For un-witnessed, the person was seen alive, and within 24 hours had died. So the data for witnessed sudden cardiac arrests is a bit more reliable. The table below displays the distribution of mean age, gender and known coronary artery disease (CAD) in those with witnessed sudden cardiac arrest.
Look at the bottom row, showing those with known coronary artery disease. Again, light activity is the main trigger. Sleep comes second. The numbers within parentheses refer to percentages within each activity group. Those percentages are not very helpful in the identification of the most important triggers, although they do suggest that coronary artery disease is a major risk factor. For example, among those who died from sudden cardiac arrest while having sex, 57 percent had known coronary artery disease. For light activity, 36 percent had known coronary artery disease.
As a caveat, it is worth noting that heavy activity appears to be more of a trigger in younger individuals than in older ones. This may simply reflect the patterns of activities at different ages. However, this does not seem to properly account for the large differences observed in triggers; the standard deviation for age in the heavy activity group was large enough to include plenty of seniors. Still, it would have been nice to see a multivariate analysis controlling for various effects, including age.
So what is going on here?
The authors give us a hint. The real culprit may be bottled up emotional stress and sleep disorders; the latter may be caused by stress, as well as by obesity and other related problems. They have some data that points in those directions. That makes some sense.
We humans have evolved “fight-or-flight” mechanisms that involve large hormonal discharges in response to stressors. Our ancestors needed those. For example, they needed those to either fight or run for their lives in response to animal attacks.
Modern humans experience too many stressors while sitting down, as in stressful car commutes and nasty online interactions. The stresses cause “fight-or-flight” hormonal discharges, but are followed by neither “fight” nor “flight” in most cases. This cannot be very good for us.
Death by running!? More like death by not running!
Reference:
Reddy, P.R., Reinier, K., Singh, T., Mariani, R., Gunson, K., Jui, J., & Chugh, S.S. (2009). Physical activity as a trigger of sudden cardiac arrest: The Oregon Sudden Unexpected Death Study. International Journal of Cardiology, 131(3), 345–349.
Good cardiology textbooks, such as the Mayo Clinic Cardiology, tend to give us a more complex and complete picture. So do medical research articles that report on studies of heart attacks based on comprehensive surveys.
Reddy and colleagues (2009) studied sudden cardiac arrest events followed by death from 2002 to 2005 in Multnomah County in Oregon. This study was part of the ongoing Oregon Sudden Unexpected Death Study. Multnomah County has an area of 435 square miles, and had a population of over 677 thousand at the time of the study. The full reference to the article and a link to a full-text version are at the end of this post.
The researchers grouped deaths by sudden cardiac arrests (SCAs) according to the main type of activity being performed before the event. Below is how the authors defined the activities, quoted verbatim from the article. MET is a measure of the amount of energy spent in the activity; one MET is the amount of energy spent by a person sitting quietly.
- Sleep (MET 0.9): subjects who were sleeping when they sustained SCA.
- Light activity (MET 1.0–3.4): included bathing, dressing, cooking, cleaning, feeding, household walking and driving.
- Moderate activity (MET 3.5–5.9): included walking for exercise, mowing lawn, gardening, working in the yard, dancing.
- Heavy activity (MET score ≥6): included sports such as tennis, running, jogging, treadmill, skiing, biking.
- Sexual activity (MET score 1.3): included acts of sexual intercourse.
What did they find? Not what many people would expect.
The vast majority of the people dying of sudden cardiac arrest were doing things that fit the “light activity” group above prior to their death. This applies to both genders. The figure below (click to enlarge) shows the percentages of men and women who died from sudden cardiac arrest, grouped by activity type.
Sudden cardiac arrests were also categorized as witnessed or un-witnessed. For witnessed, someone saw them happening. For un-witnessed, the person was seen alive, and within 24 hours had died. So the data for witnessed sudden cardiac arrests is a bit more reliable. The table below displays the distribution of mean age, gender and known coronary artery disease (CAD) in those with witnessed sudden cardiac arrest.
Look at the bottom row, showing those with known coronary artery disease. Again, light activity is the main trigger. Sleep comes second. The numbers within parentheses refer to percentages within each activity group. Those percentages are not very helpful in the identification of the most important triggers, although they do suggest that coronary artery disease is a major risk factor. For example, among those who died from sudden cardiac arrest while having sex, 57 percent had known coronary artery disease. For light activity, 36 percent had known coronary artery disease.
As a caveat, it is worth noting that heavy activity appears to be more of a trigger in younger individuals than in older ones. This may simply reflect the patterns of activities at different ages. However, this does not seem to properly account for the large differences observed in triggers; the standard deviation for age in the heavy activity group was large enough to include plenty of seniors. Still, it would have been nice to see a multivariate analysis controlling for various effects, including age.
So what is going on here?
The authors give us a hint. The real culprit may be bottled up emotional stress and sleep disorders; the latter may be caused by stress, as well as by obesity and other related problems. They have some data that points in those directions. That makes some sense.
We humans have evolved “fight-or-flight” mechanisms that involve large hormonal discharges in response to stressors. Our ancestors needed those. For example, they needed those to either fight or run for their lives in response to animal attacks.
Modern humans experience too many stressors while sitting down, as in stressful car commutes and nasty online interactions. The stresses cause “fight-or-flight” hormonal discharges, but are followed by neither “fight” nor “flight” in most cases. This cannot be very good for us.
Death by running!? More like death by not running!
Reference:
Reddy, P.R., Reinier, K., Singh, T., Mariani, R., Gunson, K., Jui, J., & Chugh, S.S. (2009). Physical activity as a trigger of sudden cardiac arrest: The Oregon Sudden Unexpected Death Study. International Journal of Cardiology, 131(3), 345–349.
Sunday, January 15, 2023
What is a good low carbohydrate diet? It is a low calorie one
What is a good low carbohydrate diet?
For me, and many people I know, the answer is: a low calorie one. What this means, in simple terms, is that a good low carbohydrate diet is one with plenty of seafood and organ meats in it, and also plenty of veggies. These are low carbohydrate foods that are also naturally low in calories. Conversely, a low carbohydrate diet of mostly beef and eggs would be a high calorie one.
Seafood and organ meats provide essential fatty acids and are typically packed with nutrients. Because of that, they tend to be satiating. In fact, certain organ meats, such as beef liver, are so packed with nutrients that it is a good idea to limit their consumption. I suggest eating beef liver once or twice a week only. As for seafood, it seems like a good idea to me to get half of one’s protein from them.
Does this mean that the calories-in-calories-out idea is correct? No, and there is no need to resort to complicated and somewhat questionable feedback-loop arguments to prove that calories-in-calories-out is wrong. Just consider this hypothetical scenario; a thought experiment. Take two men, one 25 years of age and the other 65, both with the same weight. Put them on the same exact diet, on the same exact weight training regime, and keep everything else the same.
What will happen? Typically the 65-year-old will put on more body fat than the 25-year-old, and the latter will put on more lean body mass. This will happen in spite of the same exact calories-in-calories-out profile. Why? Because their hormonal mixes are different. The 65-year-old will typically have lower levels of circulating growth hormone and testosterone, both of which significantly affect body composition.
As you can see, it is not all about insulin, as has been argued many times before. In fact, average and/or fasting insulin may be the same for the 65- and 25-year-old men. And, still, the 65-year-old will have trouble keeping his body fat low and gaining muscle. There are other hormones involved, such as leptin and adiponectin, and probably several that we don’t know about yet.
A low carbohydrate diet appears to be ideal for many people, whether that is due to a particular health condition (e.g., diabetes) or simply due to a genetic makeup that favors this type of diet. By adopting a low carbohydrate diet with plenty of seafood, organ meats, and veggies, you will make it a low calorie diet. If that leads to a calorie deficit that is too large, you can always add a bit more of fat to it. For example, by cooking fish with butter and adding bacon to beef liver.
One scenario where I don’t see the above working well is if you are a competitive athlete who depletes a significant amount of muscle glycogen on a daily basis – e.g., 250 g or more. In this case, it will be very difficult to replenish glycogen only with protein, so the person will need more carbohydrates. He or she would need a protein intake in excess of 500 g per day for replenishing 250 g of glycogen only with protein.
For me, and many people I know, the answer is: a low calorie one. What this means, in simple terms, is that a good low carbohydrate diet is one with plenty of seafood and organ meats in it, and also plenty of veggies. These are low carbohydrate foods that are also naturally low in calories. Conversely, a low carbohydrate diet of mostly beef and eggs would be a high calorie one.
Seafood and organ meats provide essential fatty acids and are typically packed with nutrients. Because of that, they tend to be satiating. In fact, certain organ meats, such as beef liver, are so packed with nutrients that it is a good idea to limit their consumption. I suggest eating beef liver once or twice a week only. As for seafood, it seems like a good idea to me to get half of one’s protein from them.
Does this mean that the calories-in-calories-out idea is correct? No, and there is no need to resort to complicated and somewhat questionable feedback-loop arguments to prove that calories-in-calories-out is wrong. Just consider this hypothetical scenario; a thought experiment. Take two men, one 25 years of age and the other 65, both with the same weight. Put them on the same exact diet, on the same exact weight training regime, and keep everything else the same.
What will happen? Typically the 65-year-old will put on more body fat than the 25-year-old, and the latter will put on more lean body mass. This will happen in spite of the same exact calories-in-calories-out profile. Why? Because their hormonal mixes are different. The 65-year-old will typically have lower levels of circulating growth hormone and testosterone, both of which significantly affect body composition.
As you can see, it is not all about insulin, as has been argued many times before. In fact, average and/or fasting insulin may be the same for the 65- and 25-year-old men. And, still, the 65-year-old will have trouble keeping his body fat low and gaining muscle. There are other hormones involved, such as leptin and adiponectin, and probably several that we don’t know about yet.
A low carbohydrate diet appears to be ideal for many people, whether that is due to a particular health condition (e.g., diabetes) or simply due to a genetic makeup that favors this type of diet. By adopting a low carbohydrate diet with plenty of seafood, organ meats, and veggies, you will make it a low calorie diet. If that leads to a calorie deficit that is too large, you can always add a bit more of fat to it. For example, by cooking fish with butter and adding bacon to beef liver.
One scenario where I don’t see the above working well is if you are a competitive athlete who depletes a significant amount of muscle glycogen on a daily basis – e.g., 250 g or more. In this case, it will be very difficult to replenish glycogen only with protein, so the person will need more carbohydrates. He or she would need a protein intake in excess of 500 g per day for replenishing 250 g of glycogen only with protein.